You are currently browsing the category archive for the ‘Awareness’ category.
Today, I just want to follow up a little about one of the points I wrote about yesterday in my post about the event I attended on Tuesday evening about diabetes-related foot complications, specifically this point made my A/Prof Ramon Varcoe:
He explored how we make people with diabetes know this technique for saving limbs is available, and said that it is really, really important to inform PWD about it so that they can ASK for it and not just accept a diagnosis of requiring an amputation. He said that this was the group that could really drive change here, by demanding that they have the best treatment possible.
This had me thinking long and hard. I agree with A/Prof Varcoe here, but that is not really a surprise. I am so much about consumer-led healthcare, that I dream about it (sad, but true).
Mostly, I thought about it in context of my own diabetes care and how it has happened that I am such a DTech nerd. I decided after about two years of living with diabetes that I wanted to use an insulin pump. I really just could not get the hang of the MDI situation I had been put on at diagnosis and was the living embodiment of why Protophane was referred to as Protopain.
I went to an information session and heard a women speaking about how much she loved using an insulin pump and what a difference it had made for her quality of life. Afterwards, I spoke with her and by the end of our chat, was convinced. I wanted one of those! (Impressionable little thing, aren’t I? #MarketersDream) This woman would become my pump trainer and the only diabetes educator I have ever seen.
At my next endo appointment, I marched in with the research I had done, the questions I needed answered and an expectation that by the end of the consultation, I would leave with details of how and when and where I would be getting my pump. Ha, the naivety!
My endo was absolutely not keen for me to take the pump road, ‘You’ve not had diabetes long enough,’ he told me, which confused me no end, because it already felt like a lifetime. ‘I think we should talk about this again after you’ve had diabetes for about 5 years. Yes?’
Well, no. That was the last time I saw him. I spent the next six months endo shopping until I found one that (I was promised) would agree to helping me on a way to a pump. I walked in and made it very clear why I was there and he nodded straight away. ‘Yep – we can do that,’ and picked up the phone. And about three months later, I was a pumper. This particular endo and I parted ways not long after because I needed someone who was far more expert in the diabetes and pregnancy track I wanted to embark, but I have always been grateful that I found him and his open attitude to diabetes technology.
When CGM was launched into Australia, I spoke to my diabetes educator and asked her to fill in the required paperwork to get me sensing. She sent the form off the day we spoke.
And the same has happened when I have wanted to change or upgrade diabetes devices.
What I am trying to say is that this has all been led by me. So when A/Prof Varcoe spoke about the importance and value of connecting with PWD and telling them about these new vascular procedures to save limbs and prevent major amputations, it made perfect sense. He urged that we needed PWD to be the ones who, if told they needed to have an amputation, spoke up and asked for a second or third opinion, specifically asking about the very procedure he had just discussed.
This ground swell of action is what causes change, but we need to know exactly what to ask for. It’s far more effective to ask the question ‘Can my artery be revascularised? I understand there is surgery than can do that and may prevent the need for a major amputation.’ rather than just ‘Is there nothing more than can be done?’
So many of the people with diabetes I know are using particular drugs or devices because they have asked for them – not because they were recommended or suggested by their HCP. And this is why PWD need to have all the information. This is why device companies should be going straight to the consumer to share information, not expecting it to happen through HCPs. (I know that there has been discomfort from some HCPs at Abbott’s direct to consumer promotion of Libre – and the fact that PWD can order themselves without needing to see a HCP, but why would that be the case?)
But it is more than just making sure the information is there for PWD to know and see. It is a complete and utter reshaping of a system that a lot of times actually isn’t about empowerment. There are still too many ‘old school’, patriarchal attitudes that dictate care choices to the PWD instead of accepting and encouraging us to lead the way for our own care. I think things are changing, but I also think they are changing far too slowly.
Last night, I heard the most amazing talk about diabetes-related foot complications. (There are words I never thought I’d write.)
Because actually, the talk was about PREVENTION of amputations. Now, I’m not talking about prevention in the sense of ‘Check your feet daily, see a HCP regularly for a foot check or if you identify problems, and wear sensible shoes’, advice I have always taken selectively. (Happy to check my feet, happy to have a HCP check my feet. But I just bought these boots…so I guess two out of three ain’t bad.) This talk was about prevention of major amputations, thanks to different surgical techniques that can save limbs.
A/Professor Ramon Varcoe, a vascular surgeon from Prince of Wales Hospital in NSW, is my new hero. I listened to his talk absolutely enthralled and amazed. Let me count the ways I adored what he said last night:
- He didn’t show gory pictures. (Thank you. Thank you. Thank.You.)
- He acknowledged that diabetes is a really difficult condition to live with.
- Furthermore, he acknowledged that those who have needed diabetes-related amputations face a really tough future.
- He explained in terms this pinhead could understand the techniques he uses to save legs from needing to be amputated. In VERY basic terms it is a technique similar to the surgery used to open arteries in the heart… a fine wire is inserted into the artery and a ‘balloon’ is used to open the artery. (He concluded his explanation by saying ‘Bob’s your uncle; we can ‘revascularise’ the limb’, making it sound so simple that anyone could do it in their kitchen on a rainy afternoon. For the record, maybe don’t do this in the kitchen on a rainy – or sunny – afternoon.)
- One way he framed his thinking was to say ‘Think of this as a ‘foot attack, the same as a heart attack’.
- He also (almost regretfully) told the audience that very few vascular surgeons perform this surgery and then went on to list the barriers: diabetes foot disease is not sexy; there is limited expertise in the filed now and learning the techniques requires retraining and great skill and there is no kudos (unlike heart surgery which does draw glory!)….Another example of the image problem that diabetes has!
- He explained that this technique is less invasive, far, far cheaper to perform, hospital stays are less, the PWD recovers much quicker, and – GET THIS! – the results are outstanding. In fact, reducing major amputations by 62%.
- He explored how we make people with diabetes know this technique for saving limbs is available, and said that it is really, really important to inform PWD about it so that they can ASK for it and not just accept a diagnosis of requiring an amputation. He said that this was the group that could really drive change here, by demanding that they have the best treatment possible. (I nearly stood up and applauded at that, but glad I didn’t because the event was at Parliament House and there were a lot of MPs and senators in the room and I was trying to behave).
- He called on better training of clinicians and campaigns to raise awareness of the procedure directly to PWD (you know – an amputations prevention initiative?!) which is exactly what we need. EXACTLTY.
- And he finished by saying: ‘My vision is for there to be no more major amputations. I hate this operation. Major amputations destroy people and destroy families. And it’s preventable.’

A/Professor Ramon Varcoe
This event was coordinated by Diabetes Australia in association with the Parliamentary Friends of Diabetes Support Group, co-chaired by Rowan Ramsey MP and Graham Perrett MP. I work for Diabetes Australia.
Just gently leaving this here today.

I am very fortunate to have a job that I truly love. But it could not be described as a particularly sexy job. At least, not the regular-day-to-day-this-is-what-I-do-when-I-am-in-the-office side of things.
I worked in recruitment for a while and the constant buzz and thrill of the game was intense. We had an old-fashioned bell in the office that would be rung when we made a particularly lucrative placement. Working on commission meant that there were dollar signs in front my eyes all the time, and I measured success in thousand dollar increments. It was sexy because it was quick, constant and there were constant wins.
Now I have a job that is what I refer to as a slow burn. Things take time, advocacy efforts are often long and drawn out, and the wins are rare. But jeez are they meaningful and worthwhile when they happen! They shoot an injection of momentum right when and where we need it, and it means we very quickly acknowledge the win and then focus on the next issue.
Sometimes people don’t realise just how long things take. When the pre-election announcements about CGM subsidies were made, a number of people commented that we’d had a busy few months to make it happen. I couldn’t help but laugh. And correct them. That particular win had been over four years of hard work.
But we take the wins were we can and this week, we’ve had a win!
The revised Assessing Fitness to Drive guidelines have been released by AustRoads and the National Transport Commission, and it’s a good news story for people with diabetes.
You may recall that there were some real issues with the previous guidelines after the completely misinformed and confusing inclusion of a definition of ‘satisfactory control of diabetes’. An HbA1c of over 9% was defined as ‘unsatisfactory control. Whilst the Commission stated that the A1c value was intended as nothing more than a guide and a trigger to seek professional care, the reality is that many people with diabetes had their licences suspended with their HCPs taking the value as a cut-off point.
As Diabetes Australia consistently argued, there is no evidence to suggest that an elevated A1c makes a person with diabetes more dangerous on the roads. In fact, this focus on an elevated A1c was actually detracting from hypoglycaemia, which is something that does need to be considered.
In the new guidelines, the number has been removed which is an excellent outcome for PWDs. And added to the document is far more focus on impaired hypoglycaemia awareness and keeping safe on the roads.
This change didn’t happen because we asked nicely. In fact, it took four years – from when the last guidelines were launched and we started to hear of people with diabetes having troubles – for the change to be made.
It took a lot of advocacy: letter writing, speaking with people who had been negatively impacted, meetings and teleconferences, and revising documents.
This is what I mean when I say that my job is unsexy. All of the work that was done behind the scenes – the slow burn – is decidedly unsexy! But it has to be done to get the wins.
I’ll admit to doing a very quick victory dance when I heard about this particular win. But the celebrating didn’t last long.
Because there is so much more unsexy work to do. Until people with diabetes are no longer discriminated against; until diabetes stigma is something we only speak about in the past tense; until kids with diabetes in schools are freely given all the same opportunities as their peers who make their own insulin; until access – to drugs, technology, healthcare – is available to all, the unsexy stuff will keep happening. You probably won’t hear about it until there is good news, but the wheels keep turning and the fire keeps burning slowly. As I said in this post here, it’s the reason I do what I do.
The new Assessing Fitness to Drive guidelines can be downloaded here.

Four years ago in Rome, I made Aaron take a photo of me with just about every old Fiat Cinquecento we saw. There are a lot of photos of me with tiny cars!
Disclosure
I was a representative on the Diabetes Working Group revising the diabetes chapter of the new Guidelines. This was part of my role at Diabetes Australia.
If you have not caught up with what happened in the opioid session at MedX this week, please do. ePatient, Britt Johnson, who blogs at Hurt Blogger wrote this outstanding piece about her experience on the panel in a session titled ‘The Opioid Crisis’ where she was pretty much ignored by the moderator of the panel. I read her piece in dismay because Britt’s experience is all too common.
As I wrote on Facebook yesterday, it is these twelve words of Britt’s post that are, for me, most telling:
‘The plan had been to feature me in the final five minutes.’
This was the response from the moderator of the panel when she was challenged as to why Britt has been ignored whilst on stage.
The final five minutes.
That’s right. After the healthcare professional experts got to say what they wanted; after the moderator directed the discussion in a direction to get what she wanted; after everyone but the patient was given an opportunity to speak. Then, and only then, would Britt have been given the opportunity to say what she wanted.
The final five minutes.
It’s the equivalent of being given a completed resource, almost ready to go to print and being asked to provide feedback. It’s the same as being a perfunctory consumer on an advisory board, often added at the last minute to tick a box.
This token and downright insulting attitude about where ‘patients’ fit into the healthcare puzzle is toxic.
We have become accustomed and too accepting of the status quo. We feel humbled when we are added to a panel discussion when, really, we should be the main event. We are honoured to be asked to provide feedback on an already developed service that we are meant to use because we mistakenly believe our opinion is being sought and matters even though it’s too late for our feedback to be taken on board. We believe we are doing well when a consumer is added to an advisory board made up predominantly of clinicians and researchers because, hey, it’s a start.
A start is not good enough anymore.
I am angry. I am so angry about this. I am angry about what happened to Britt at MedX. I am angry that there was not a single person with diabetes on the program at this year’s ADS ADEA conference. I am angry that it is 2016 and we still have to beg for a place at the table, on the panel, on the Board. I am angry that conversations ABOUT us are happening AROUND us. I am angry because there’s never a hesitation then it comes to convening a clinical advisory group, but a struggle with how and where to engage and appoint a consumer advisory group. I am angry because too many think ‘focus testing’ means engaging at the end, and that it is enough.
But mostly, I am angry at myself. I am angry for this post I wrote last year where I pathetically felt grateful because people with diabetes were quoted at a conference – not actually handed a microphone, not actually invited to sit on a panel, not given an opportunity to lead the discussion. We were quoted and I thought that was enough.
It was our final five minutes. And, actually, it wasn’t enough.
We are more than the final five minutes.
We are more than that; we are so, so very much more.
Apparently, I went to Munich. I was away for 6 days, and 60 hours of those days were spent in transit. I believe that, (as I deal with jet lag, hypoglycaemia, and mainlining caffeine), it is fair and accurate to say that I am too old for this shit.
I am also incapable of forming paragraphs. But dot points are fun! Here are some observations and a few silly thoughts from last week. (I’ll write some sensible things when my brain is back in the same country as the rest of me.)
- I am told by people Munich is a lovely city. I will have to take these people’s word for it, ‘cause I saw very little of the city.
- I did not buy a dirndl and for this, I will be eternally sorry. As will my husband.
- The EASD conference itself was, as predicted, very rats and mice-y. I sat in a number of sessions and wished I was a mouse (while wishing my diabetes away). Alas, I am not a mouse. And I still have diabetes. Damn.
- I did not get sick of laughing at the fact that one of the halls at ICM Messe München is called Langerhan Hall. Also, I did not get sick of saying ‘I wonder if my islet cells are in there’ – to everyone within earshot. Even if I didn’t know them.
- Obviously, Grumps was not as amused by this as me.

- As was the case at ADA, my arm is more recognisable and famous than me. A barista at one of the exhibition hall stands said, as making me a decent coffee, ‘Oh – I know you. I saw your arm the other day near the station.’ I am a walking billboard for Rockadex! (I am not sponsored by Rockadex and purchase my own patches.)
- Dr Kevin Lee from Queensland is a tweeting machine! In fact, I think the thing I was proudest of at EASD was seeing him tweet! (Actually, probably should say that Professor Mark Cooper’s giving the Claude Bernard Lecture was also a moment of national pride, but Kevin’s tweeting was on another level!)

- One of my favourite talks was about diabetes, cardiac health and exercise (go on, laugh….), but that was mostly because presenter Dr Nikolaus Marx, finished up with a discussion about passive exercise and cardiovascular events during the World Cup. If you were in the room, it was me who cheered when he mentioned the increase of cardiac events after Italy beat Germany. (#VivaItalia!). For clarification, I was cheering at Gli Azzuri’s victory, not the number of Germans having heart attacks. (By the way, this was a real study. Published here.)
- A HUGE shout out to these three women. AADE presidents elect, past and present, Nancy D’Hondt, Deb Greenwood and Hope Warsaw are absolute advocates for and champions of people with daibetes, and peer support. This is them at the docday blogger and advocate event. This level of commitment by HCPs to consumer engagement is enlightening, and a lot could be learnt from their example here. Thank you. Thank you. Thank you!

- It was wonderful to see quite a lot of discussion about AP. Anytime someone wants to actually get these into market and into the hands of people with diabetes, that would be just great! Thank you.
- I may have screamed a little when I wandered through the Association Village to the excellent historical display of diabetes by the German diabetes Association. Terrifying might be the word for these needles. I said a little prayer of thanks to the diabetes angels for modern day tech, and for being diagnosed in 1998.

- I need to take a break from twitter. This was the state of play when I said good bye to the conference.

And finally, a word about language, because I am unable to attend a conference and not talk and write about it. (I think it’s actually become a law somewhere.) This probably deserves a post of its own and that may happen, but here we go anyway.
This is the fifth EASD conference I have attended, and going in, I know that it is going to be challenging, language-wise. There often appears to be very little consideration that there could be PWD in the room listening in to how HCPs are speaking of us. In the opening ceremony, I tweeted this at EASD president, Professor Juleen Zierath:

I was a little disappointed at Professor Mark Cooper’s constant use of ‘diabetic’, but it was by no means any more than most of the other speakers. I suppose I just hold Australian speakers to higher account given the work we have been doing here around language and diabetes.
This tweet generated quite a lot of discussion, and came about after I was exhausted and annoyed and mostly frustrated by the way speakers were referring to people with diabetes.
 Perhaps the best response was from Nick Oliver:
Perhaps the best response was from Nick Oliver:

Here’s the thing – and it is something I spoke about during my talk at the DOCDAY event. Language DOES matter. We all know that. It’s completely and utterly disingenuous to say it doesn’t. For some people, it doesn’t bother them and that’s terrific. For others, though, it really does. So why would anyone do something that may offend when it is so easy to avoid that?
DISCLOSE DISCLOSE DISCLOSE
My (economy fare) flights and accommodation expenses were covered by AMSL and J&J. I was attending the EASD conference mainly to attend the J&J DOC exchange meeting which I was involved in preparing and presenting. No one ever expects me to write anything. These are my words and observations only. (And seriously, have you seen what I have just written? No one wants to be associated with that!)
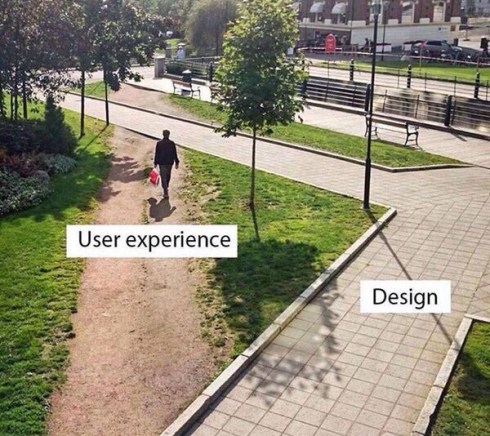
This photo* sums up why I do what I do, and why many people think I sound like a broken record, with a vocabulary of a mere seven words. Specifically, these seven words: ‘Have you spoken to people with diabetes?’
Because so often, the answer is ‘No’. Or ‘No – we’ll be doing that after we have had some meetings.‘ Or ‘Yes – we spoke to you‘ at which point I remind them that I pointed out when they did indeed speak to me that they should find other people with diabetes to speak with. Because I am but one person and speak for no one other than me. (Or, perhaps, another woman in her 40s who loves Nutella, boots, coffee, lives in inner-Melbourne, waves her hands around madly while speaking reallyreallyreallyreally fast, can recite Marx Bros movies from start to end, has what some would call an irrational fear of birds (and butterflies), can sing (badly) pretty much any song from the 1980s, has over 25 striped t-shirts in her cupboard and is battling an eleven year old daughter who has decided that she too loves stripes and wants to borrow all her mother’s clothes.)
Most people are not like that. (Fortunately.)
Anyway, this picture also demonstrates that those who have the privilege of designing services, activities, programs, settings for people with diabetes often miss the point – perhaps not by much, but nonetheless, they miss it. It’s usually because they forgot to ask us, or asked as too late, or didn’t keep coming back and asking and checking in. And then, when we don’t use what they design, we are branded ‘non-compliant’ or ‘disengaged‘ or ‘not interested in our health’, when the truth of the matter is that their design (without our input) just doesn’t fit our needs.
I have given so many talks and written so many pieces about this. But perhaps all I need is this on a t-shirt, tattooed to my arm (forehead?) and on the back of my business cards. Don’t design before speaking to the user. It’s actually really easy!
(*I don’t know the source of this photo, but if anyone does, please let me know so I can credit appropriately.)















