You are currently browsing the category archive for the ‘Real life’ category.
Our kidlet is starting secondary (high) school next year. Her parents are totally in denial about this – we keep looking at photos of her from five or six years ago, pretending she is only in her first years of primary school. This works perfectly until we actually look at her today – tall and lanky and tweenager-y – and realise that denial can only take us so far!
The other night, we attended an orientation evening at her new school. As we were rushing about getting ourselves organised and out the door to get there on time, I was mainlining water and continuing to rage bolus my way through awfully high glucose levels. The throat infection I’ve had for a couple of weeks seemed worse and was absolutely kicking my arse. Apart from a milky coffee in the morning, I’d had no carbs all day, and yet each time I looked at my iPhone for my CGM number I was furious.
At one point, I blinked away tears as I saw another number in the high teens and a stubborn, perfectly-straight CGM trace that was stuck in the yellow zone of the graph.
My mantra of ‘it’s just a number’ wasn’t cutting it. The razor-blades in my throat were agonising and my legs and arms were achy – a combination of a low-grade fever and high-grade molasses pulsing through my veins. I threw back a couple of Nurofen, chugged a large glass of water and we piled out the door and into the car.
We got to the school and the kidlet found one of her friends and we all settled in the beautiful school library, waiting to hear about the school’s transition program and what our kids could expect as Year 7 students next year.
The move to this new environment is made as smooth as possible for the students, however there was a lot of acknowledgement from the Principal and the year level coordinator that it would be different and challenging time, as well as a chance for some terrific opportunities.
The Principal said some really soothing and encouraging words – for the benefit of both the new students and their equally (perhaps more?) anxious parents. It was lovely to hear about the supportive and inclusive environment on which the school prides itself, and the initiatives and activities they undertake to help the students become part of the school community.
But the words that struck me most and made me think that we had made a really good decision about this particular school came when he was speaking about exams, tests and assessments.
He acknowledged that getting results for assessments can be a little nerve-wracking at times and that it is perfectly normal to feel some level of anxiety. And then he said ‘But a result is just a snapshot in time. It does not determine where you are going.’
I looked over at our girl then and saw her listening intently. She has heard us say similar things before in relation to school tests and she has heard me say it a lot of times in relation to diabetes numbers.
As the Principal continued talked about the school, I stole a look at my phone for my CGM and saw the number 19.6 looking at me. I recognised the anxiety I had been feeling earlier was two-fold: anger at being high and the lousy feeling that comes with it. But also the fear of high numbers as a long term problem. Subconsciously, the inextricable link between high numbers and complications lurks, littering my mind with fear.
It doesn’t matter how much I know about complications and improvements in management, that fear is always there. I know about how much better the outcomes related to complications are these days for people with diabetes when compared with ten, twenty, forty, fifty years ago – I still am terrified. And never more so than when I am high.
I took a deep breath and returned my phone to my handbag. In my head I repeated the words the Principal had just said a few moments earlier and felt myself breathing easier. ‘It’s just a snapshot in time. It does not determine where I am going.’ I said it again. And again. And again. Until I almost started to believe it. Almost.

Unpleasant
Trying to make sense of the weird link between visiting old family homes, coffee, and searching for security and safety in diabetes. Sometimes, my thought process is ridiculous!
‘Oi!!!!’
‘Hey!! Hey!! Oi!!’
I have a particular look that I reserve for men who yell at me from passing cars. Admittedly, this look is employed far less frequently than when I was a younger lass, but occasionally, it still does need to be used.
And today, the thunderous look of complete and utter disdain was on my face, and the choice words I was going to use to accompany it were forming on my lips as I turned to the person who was shouting at me from their car which was actually stopped at a set of lights as I crossed the road in front of it.
It took me a moment to realise what was going on, but there was a man, half leaning out the window of the passenger side of the car, flailing his arms around and, once he had my attention, yelling ‘Look!!! Look!!!’
I looked.
And there, on his arm, he was sporting a CGM. Just like me – mine circled by a dark blue RockaDex patch; his with a bright green one.
I jumped up and down (by this time I had safely crossed the road) and yelled back. ‘Oh my god!!!! Hey!!! Hey!!! We are totally best friends now!!!’ I was waving my arms around as well, absolutely not caring how ridiculous I looked.
The lights changed and the car took off. He gave me a last smile and yelled good bye. And I waved at the car, standing there on the side of the road, laughing out loud.

Today, I just want to follow up a little about one of the points I wrote about yesterday in my post about the event I attended on Tuesday evening about diabetes-related foot complications, specifically this point made my A/Prof Ramon Varcoe:
He explored how we make people with diabetes know this technique for saving limbs is available, and said that it is really, really important to inform PWD about it so that they can ASK for it and not just accept a diagnosis of requiring an amputation. He said that this was the group that could really drive change here, by demanding that they have the best treatment possible.
This had me thinking long and hard. I agree with A/Prof Varcoe here, but that is not really a surprise. I am so much about consumer-led healthcare, that I dream about it (sad, but true).
Mostly, I thought about it in context of my own diabetes care and how it has happened that I am such a DTech nerd. I decided after about two years of living with diabetes that I wanted to use an insulin pump. I really just could not get the hang of the MDI situation I had been put on at diagnosis and was the living embodiment of why Protophane was referred to as Protopain.
I went to an information session and heard a women speaking about how much she loved using an insulin pump and what a difference it had made for her quality of life. Afterwards, I spoke with her and by the end of our chat, was convinced. I wanted one of those! (Impressionable little thing, aren’t I? #MarketersDream) This woman would become my pump trainer and the only diabetes educator I have ever seen.
At my next endo appointment, I marched in with the research I had done, the questions I needed answered and an expectation that by the end of the consultation, I would leave with details of how and when and where I would be getting my pump. Ha, the naivety!
My endo was absolutely not keen for me to take the pump road, ‘You’ve not had diabetes long enough,’ he told me, which confused me no end, because it already felt like a lifetime. ‘I think we should talk about this again after you’ve had diabetes for about 5 years. Yes?’
Well, no. That was the last time I saw him. I spent the next six months endo shopping until I found one that (I was promised) would agree to helping me on a way to a pump. I walked in and made it very clear why I was there and he nodded straight away. ‘Yep – we can do that,’ and picked up the phone. And about three months later, I was a pumper. This particular endo and I parted ways not long after because I needed someone who was far more expert in the diabetes and pregnancy track I wanted to embark, but I have always been grateful that I found him and his open attitude to diabetes technology.
When CGM was launched into Australia, I spoke to my diabetes educator and asked her to fill in the required paperwork to get me sensing. She sent the form off the day we spoke.
And the same has happened when I have wanted to change or upgrade diabetes devices.
What I am trying to say is that this has all been led by me. So when A/Prof Varcoe spoke about the importance and value of connecting with PWD and telling them about these new vascular procedures to save limbs and prevent major amputations, it made perfect sense. He urged that we needed PWD to be the ones who, if told they needed to have an amputation, spoke up and asked for a second or third opinion, specifically asking about the very procedure he had just discussed.
This ground swell of action is what causes change, but we need to know exactly what to ask for. It’s far more effective to ask the question ‘Can my artery be revascularised? I understand there is surgery than can do that and may prevent the need for a major amputation.’ rather than just ‘Is there nothing more than can be done?’
So many of the people with diabetes I know are using particular drugs or devices because they have asked for them – not because they were recommended or suggested by their HCP. And this is why PWD need to have all the information. This is why device companies should be going straight to the consumer to share information, not expecting it to happen through HCPs. (I know that there has been discomfort from some HCPs at Abbott’s direct to consumer promotion of Libre – and the fact that PWD can order themselves without needing to see a HCP, but why would that be the case?)
But it is more than just making sure the information is there for PWD to know and see. It is a complete and utter reshaping of a system that a lot of times actually isn’t about empowerment. There are still too many ‘old school’, patriarchal attitudes that dictate care choices to the PWD instead of accepting and encouraging us to lead the way for our own care. I think things are changing, but I also think they are changing far too slowly.
I had a low last week that knocked me for six. It certainly wasn’t the worst hypo I have ever had – far from it actually. But it had been a while since I had one like this. In fact, since I started eating low(er) carb. (I’m still reluctant to call it low carb, because I am really not trying to stick to a certain amount of carbs per day. But to give you an idea, it’s a rare day that I eat more than 80 grams.)
But last week, I did. My usual Japanese food takeaway place was out of sashimi which is my favourite quick lunch. So, I ordered a sushi roll and a cup of miso and off I went.
Now white rice is evil to me. It really is. I love it, but have never managed it! In 18 years of type 1, I have never worked out how to bolus for it. I am better (although not great) with pasta and other carb-heavy foods. But rice? Just hopeless! I would just guess, hope that I was close to right and then kept a close eye on my numbers afterwards, correcting as necessary.
On Friday, I was nowhere near right. No.Where. I watched my CGM line start to rise and rise and rise pretty quickly after I ate, resisting the urge to bolus before I hit the upper limit on my graph. And I am so glad I didn’t because after the spike, came the plummet. Insulin still on board, and two arrows pointing down.
I tried to intervene, but it was too late. Suddenly, my lips starting tingling, I realised I was sweating a lot and my thought process was all over the place. I read the same email five times, started five different responses and had no idea what I was trying to say.
I grabbed a juice box, and drank the lot in one gulp. The desperate low feeling of ‘I.Am.Going.ToDie’ overtook me as I stabbed another straw into another juice box and looked around for what else I could consume that would help, grabbing a handful of jellybeans; spooning honey from the jar and pouring some milk into a bowl with cereal.
And then I stopped. I willed myself to breathe, counting up as I inhaled, down as I exhaled, trying to not get the numbers messed up. I concentrated on my heartrate. I walked away from the food on the kitchen counter and sat at the table, focusing on the artwork above the wood-fire oven that the kidlet and I had done years ago when she was only about 5 years old. I thought about us spreading down a drop sheet on the front veranda of our old house, sitting the large canvas on top of it and emptying tube after tube of paint onto it. ‘It’s like a Jackson Pollock painting,’ she said, signing the finished artwork with her name and then adding ‘and Mummy’ afterwards.
Slowly, my heartbeat returned to normal. I could count my breathing without difficulty. I stopped thinking that I was going to pass out. My clothes were drenched from the sweating, though and now I was shaking because I was cold. I gingerly walked into the bedroom, pulled off my top and put on a thick jumper, wrapping a scarf around my neck for good measure.
I looked at my CGM graph on my iPhone and saw the quick spike and the sudden crash – a sight I’d not seen for some time. I lay down on my bed and closed my eyes for a moment, which became an hour and when I woke, the ‘hit-by-a-bus’ hypo hangover had taken over my body.
All this because of a sushi roll gone wrong. It wasn’t even a delicious doughnut or cupcake, I thought. It took me almost 24 hours to get back on track. The over-treating had to be corrected and I tried to not over correct, but that failed and another low in the middle of the night messed me up a little more.
This was a forgotten low. And I’m not particularly inclined to have another one in the near future to remind me again.

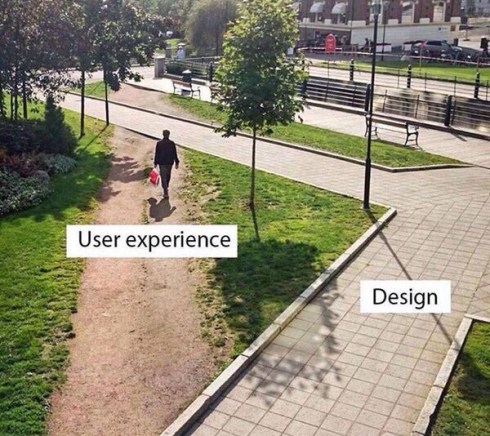
This photo* sums up why I do what I do, and why many people think I sound like a broken record, with a vocabulary of a mere seven words. Specifically, these seven words: ‘Have you spoken to people with diabetes?’
Because so often, the answer is ‘No’. Or ‘No – we’ll be doing that after we have had some meetings.‘ Or ‘Yes – we spoke to you‘ at which point I remind them that I pointed out when they did indeed speak to me that they should find other people with diabetes to speak with. Because I am but one person and speak for no one other than me. (Or, perhaps, another woman in her 40s who loves Nutella, boots, coffee, lives in inner-Melbourne, waves her hands around madly while speaking reallyreallyreallyreally fast, can recite Marx Bros movies from start to end, has what some would call an irrational fear of birds (and butterflies), can sing (badly) pretty much any song from the 1980s, has over 25 striped t-shirts in her cupboard and is battling an eleven year old daughter who has decided that she too loves stripes and wants to borrow all her mother’s clothes.)
Most people are not like that. (Fortunately.)
Anyway, this picture also demonstrates that those who have the privilege of designing services, activities, programs, settings for people with diabetes often miss the point – perhaps not by much, but nonetheless, they miss it. It’s usually because they forgot to ask us, or asked as too late, or didn’t keep coming back and asking and checking in. And then, when we don’t use what they design, we are branded ‘non-compliant’ or ‘disengaged‘ or ‘not interested in our health’, when the truth of the matter is that their design (without our input) just doesn’t fit our needs.
I have given so many talks and written so many pieces about this. But perhaps all I need is this on a t-shirt, tattooed to my arm (forehead?) and on the back of my business cards. Don’t design before speaking to the user. It’s actually really easy!
(*I don’t know the source of this photo, but if anyone does, please let me know so I can credit appropriately.)
There are few topics guaranteed to polarise and cause debate like food and what we are eating. Our choice of what we put in our mouths will always generate comments, whether invited (and welcome) or not. And add diabetes to the mix and it gets even worse. From ‘Should you be eating that’ to ‘Here, this is low fat, low sugar, high cardboard content’, we get it all!
I wrote a couple of months ago about how I had unintentionally started eating low(er) carb, and shared my thoughts on how that was going. I’ve also made a few comments on my social media feeds about some things I’d been trying. Interestingly, and as a result, I’ve been contacted by complete and utter strangers wanting to give me their thoughts. This in itself is not that odd; I frequently have messages from people I don’t know about my blog.
What is different here though, is the tone that is often used. And it is not always particularly positive. I’ve been accused from jumping on a bandwagon, loving Pete Evans (that one made me laugh for about four days straight!), letting down the team and being untrue to my Italian heritage. I ignored them all.
I’m a few months in now and couldn’t really care less what people think. I am trying something to try to improve my own diabetes management, not anyone else’s and I’m certainly not even considering suggesting that this is something others might like to try. The My Diabetes My Rules thing possibly applies here more than anywhere else.
The experiment has been continuing, and what I have been most interested in is not only the results regarding my diabetes, but I also really wanted to know if this change in my hearting habits is truly sustainable.
So, a couple of things I want to say to begin with. I have not adopted low carb high fat as a way of life for me. I am ad hoc at best. There are some things that I refuse to change and I have no problem with that at all. This lack of real commitment has drawn criticism from a few people who also thought they would message me to say that if I wasn’t doing low carb high fat properly that I was a fraud and should just shut up. I ignored them too. (That’s the beauty of writing your own blog – you don’t have to listen to people!)
The sustainability issue seems to have worked for me by muddling through the best way I can, making sure that I never say no to something I really want to eat. And perhaps, that was the ‘Aha’ moment for me. There is no right way to do this – except the way that works for me.
For example: I love bread. Love it. Adore it. Love. Love. Love. But there is bread and there is bread. When I eat bread, I only eat bloody good bread. Like a beautiful, chewy seeded sourdough from Baker D Chirico, bought fresh from the bakery and slathered with lashings of real butter – preferably French; always salted.
I’ve decided that there is no point eating a piece of highly processed square bread out of a packet that is not freshly baked and is full of preservatives. So I don’t eat it.
My breakfast most mornings continues to be a milky coffee. I’m nor cutting out the milk or the sugar, even though I know both do raise my BGLs. But I manage that as well as I can, hoping for no spike within half an hour of consumption. I am not good in the mornings without that first (and often second) coffee. And for the love of all that is good and those around me, it’s best that I just have my latte and get on with it.
Overcoming the mindset of needing to eat carbs has been a huge challenge for me. HUGE. It is possibly a combination of 18 years of conditioning about the need to include carbs in my meals and also generally loving carb-based foods.
But there are options. And as I work out what they are, meals are becoming easier.
Where I think I have been getting the biggest bang for my buck is adapting evening meals to be lower carb. This has resulted in far nicer glucose levels in the evenings, overnight and, subsequently, in the mornings. For me, it’s complete
ly and utterly undeniable that not loading with carbs equals diabetes that is far easier and nicer to try and manage.
 So, here are just a few things that I’ve prepared recently to give you an idea of what I have been doing to lower my carb intake. Often, my evening meal is zero carbs which is generally what I have been aiming for as this offers the best post-prandial results.
So, here are just a few things that I’ve prepared recently to give you an idea of what I have been doing to lower my carb intake. Often, my evening meal is zero carbs which is generally what I have been aiming for as this offers the best post-prandial results.
For the colder months, the oven has been working overtime, cooking braises and stews for hours at a time. Or one pan wonders like this that combine chicken, chorizo, lemon, garlic and spinach.
 I always love to serve them with mashed potatoes, but have tried mashed cauliflower instead. I refused to even entertain the thought of mashed cauli until recently, when I decided to try it and have found it it delicious. (I either steam or bake it first
I always love to serve them with mashed potatoes, but have tried mashed cauliflower instead. I refused to even entertain the thought of mashed cauli until recently, when I decided to try it and have found it it delicious. (I either steam or bake it first
and then pulverise it with a stick blender with salted butter (lots) and milk. Or cream if I have some in the fridge.) I can eat a huge bowl of it and my glucose levels do not shift a smidge. (I know this to be true because I have, on several occasions, eaten nothing but a huge bowl of it for dinner and then watched the flat line of my CGM.)
 Actually, cauliflower has become a favourite food. And it’s insanely cheap at the moment. Roasted cauli has become another staple. My favourite way is to cut out the core and bake it whole, drizzled with olive oil, oregano and fresh garlic. But cauliflower is one of those veggies that simply soaks up flavours, so anything goes. I’ve also tried lemon, garlic and rosemary which works a treat. (I’ve worked out that steaming the cauli in the microwave for about 5 minutes first cuts the cooking time down, so usually I do that before shoving it in the oven.)
Actually, cauliflower has become a favourite food. And it’s insanely cheap at the moment. Roasted cauli has become another staple. My favourite way is to cut out the core and bake it whole, drizzled with olive oil, oregano and fresh garlic. But cauliflower is one of those veggies that simply soaks up flavours, so anything goes. I’ve also tried lemon, garlic and rosemary which works a treat. (I’ve worked out that steaming the cauli in the microwave for about 5 minutes first cuts the cooking time down, so usually I do that before shoving it in the oven.)
I made low carb gnocchi one night with hazelnut meal instead of flour and tossed them through a burnt butter and sage sauce, with tiny pieces of crispy fried pancetta sprinkled on top.

Do I feel as though I missing out on anything? Not really. Because if I want something, I still eat it. No foods are considered taboo, there are still no ‘good’ or bad’ foods. I still bake heaps and sample everything I make. (Case in point – these amazing squidgy choc-chip cookies I made the other day that are delicious!)
But what I do know is that minimising riding the blood glucose rollercoaster makes me feel better and this is by far the easiest way I have ever known to do that. It’s not perfect and there are still un-explained highs and lows. There is no name for this way of eating. But it is working for me, so for now, I’ll stick to it.
There is a dance I do with diabetes each and every day. I praise, celebrate and highlight the good; I avoid, shut out and ignore the bad. The things that scare me are pushed away – as deep as they can go. When they threaten to rise to the surface, I do the equivalent of sticking my fingers in my ears and start chanting ‘la, la, la’ so they recede to where they belong. Out of sight. Out of mind.
I’ve done this for as long as I’ve had diabetes. From day one, I pushed away the ugly and scary images of diabetes complications. I conveniently ignored the warnings and threats. Obviously. Because no one wants to be scared or warned or threatened the day they find out they have a life-long chronic health condition. Or ever.
I am scared. Diabetes scares me a lot. It always has, but for some reason, it is more at the moment. I don’t know why. Nothing has changed. There has not been a frightening experience or a noticeable change in anything. But as days and weeks and months and years as a person with diabetes gets crossed off some imaginary calendar, I am suddenly feeling that it is a countdown to where the really difficult things start.
I worry about what each passing hour is doing to my body and to my mind. If I’m being particularly forgetful, I wonder if it is because my head is so full of diabetes considerations that there is no room for a synonym for fear (dread, anxiety, terror, dismay alarm….) or recalling what day my kid has library each week.
But thinking about it more, I think the fear comes from the lies we are sold about our diabetes. I was promised the day I was diagnosed by a lovely, but most likely completely out of touch doctor, that diabetes is a matter of maths and that if you do the equations properly, it can be easily controlled.
Diabetes can’t be controlled, and with each moment of failure – and there are many and they are constant – I have feared the consequences. And I fear diabetes. With each missed calculation or out-of-range number or confusion about how the hell this thing really works, I see failure. And fear.
Diabetes is not a matter of maths, and the idea that I can control it results in a constant state of high alert as I pretend to be a body part that, when working, is pretty damn perfect. I am not perfect. In any way. And neither is the way I manage my diabetes. It’s messed up. And I’m messed up about it.
And now, as always, there are the fears. And they seem bigger and bolder all the time. I fear diabetes-related complications – long- and short-term. I fear losing the ability to take care of myself and care for others. I fear diabetes becoming so intrusive that I am unable to do anything else. And I fear diabetes becoming the first, last and only thing others think about when they see me. Perhaps most of all, I fear diabetes becoming the first, last and only thing I think about when I see me…
I wonder just how differently I would feel about diabetes – the known and unknown – if I was told at diagnosis that I would get this wrong more times than I got it right. And that was perfectly okay, understandable and acceptable. I wonder how much less significant the feelings of failure would be. And how much more in check my fears would be.

9 March, 1998. 37 days before diagnosis.
My first car was a 1970s Fiat 128. It was bright yellow (‘limone’) and was my pride and joy. It cost me under $2,000 back in 1993 and it remains the coolest car I have ever driven.
I longingly think back to the days of driving around in a little zippy car that was bright and fun. Other Fiat drivers would toot their little horns when they saw me on the road, and I would raise my hand in a friendly wave of vintage-car solidarity.
But it was very basic. There was absolutely nothing fancy about this car. In fact, today, it would struggle to pass a road-worthy check.
I had to keep a little container of spare fuses in the glove box because the electrics were shot. When it rained, the wipers would stop working. (Useful, I know!) As water leaked through the bonnet and onto my shoes, the wiper fuse would blow after sparking dramatically. I became incredibly efficient at reaching over and into the glove box stash for a new fuse, removing the dead one from the fuse box located just under the steering wheel, and replacing it with one that would get my wipers swiping again. All while continuing to drive through the rain, squinting through the water droplets on the windscreen until the wipers sprung back into action and I could see properly again.
Oil needed to be checked daily as it would frequently leak from the engine, and I was terrified of blowing the head gasket if I let the oil tank run dry.
The speedometer read in MPH, so I had used specks of Liquid Paper to mark 60kms and 100kms in a lame endeavour to remain within the speed limit – something that I only did rarely anyway.
I developed enviable muscles in my upper arm steering the little thing because power steering hadn’t been invented when this car was built.
And, of course, it was a manual car, because automatic cars were for wimps who didn’t know how to drive. This idea was beaten into me by my cousins who taught me to drive on the winding Kew Boulevard near home with no instructions other than ‘Don’t brake around corners. And don’t go below 60KPH’. I learnt to drive with the attitude and confidence of a Roman taxi driver.
I grew up being driven around in Fiats and Lancias. Even now, my dad drives an Alfa Romeo. So does my sister. And most of my extended family. These days, when I drive up to family gatherings in my sensible German-made car, they look at me with pity, and then turn away as they continue to look at their stylish reflections in the stylish windows of their stylish Italian cars.
The kidlet has already decided that her first car will be a Fiat Cinquecento in pale blue. I think she is ashamed and embarrassed to be seen in my boring and decidedly uncool silver Merc, preferring a zippy little Italian number so she can legitimately shout obscenities at cars driving too slow on the road while waving her hands at them. (#HerMothersDaughter)
These days, I drive an automatic car that pretty much does everything for me. It alerts and alarms and warns me if there is anything likely to interfere with my driving. It reminds me when it needs servicing, and is easy as easy to drive. Everything is programmed and instinctive, and perfectly set out, in brilliant, efficient, modern and safe German order.
In fact, my car today operates much like the diabetes tech I use: the latest equipment; the most efficient. I was an early adopter of pump therapy, one of the first people to start using CGM here in Australia, and have always liked to have the newest and snazziest BGL meter in the little Marimekko purse in my handbag.
I have no sentimental feelings towards any of my tech – I’m more than happy to ditch whatever I am using as soon as something newer, faster, brighter, smarter comes along.
I can’t for a moment imagine wanting to go back to using diabetes tech from 1970 (was there any diabetes tech in the 1970s?), but the thought of my mid-seventies Fiat makes me swoon. It was also a time before diabetes. Maybe the rose coloured glasses that are firmly placed on my face when thinking about my Fiat, also reflect a time when I didn’t need technology to keep me alive.
The other day, I saw a little yellow Fiat like the first one I owned. They are pretty rare these days and I get incredibly excited when I see one. I was in my car, stopped at a set of lights, and there, in my perfectly aligned, safety-glass rear-view mirror, I saw a flash of yellow. The Fiat pulled up next to me on the passenger side of my car. There in the driver’s seat was a woman about my age. She looked over at me and I smiled.
I flashed back to being 19 years old, driving around Carlton feeling like the coolest kid ever, without a care in the world. I didn’t have to think or worry about diabetes then. I didn’t have to check my BGL before starting the engine. Or make sure I had a supply of hypo foods hidden away. I didn’t have to wonder if I was going low on a long trip and pull over and check my glucose levels to make sure I was safe to keep driving.
In fact, the only thing I had to check before I got in the car was that I looked sharp and cool. Oh and that I had enough fuses in the glovebox for the fifteen-minute drive to Uni!

22 years ago! My gorgeous little Fiat 128. And me looking like an extra from ‘Friends’ in my 1990s jeans!




















